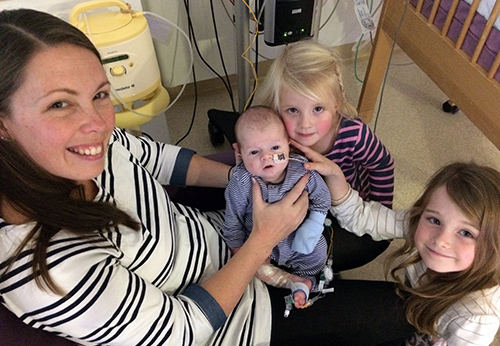
Pictured: Jake with mum Rebecca and sisters Alexia and Isabella on the Neonatal Intensive Care Unit
A mum whose baby was born at full-term but ended up fighting for his life in the Neonatal Intensive Care Unit (NICU) at the Lancashire Women and Newborn Centre wants to spread awareness that it’s not just tiny, premature babies that are born poorly.
Rebecca Crompton, 34, who lives in Blackburn, is full of praise for all the care and support her baby son Jake received at East Lancashire Hospital’s NICU based on the site of Burnley General Teaching Hospital.
Rebecca, who is married to Jonathan, was actually past her due date when she gave birth to baby Jake Crompton and he was born at 41 weeks weighing 8lbs 4oz.
Rebecca, a primary school teacher in Accrington, who also has daughters Alexia, eight and Isabella, four, says: “My first little girl was born nine weeks early so if anything, I was more prepared for Jake being premature than overdue.”
Everything went smoothly during Rebecca’s pregnancy and when she went into labour, she went to have Jake at Blackburn Birth Centre where she had her second daughter Isabella and had a really positive experience using a birthing pool and wanted the same again.
Rebecca says: “I was progressing well but then I got to six or seven centimetres dilated and just could not get Jake to move.
“I got out of the birthing pool and they tried me in all sorts of different positions and then they realised the baby’s heart rate had dropped.”
Rebecca had an episiotomy to get Jake out quickly and when he was born, he was blue and not breathing so had to be resuscitated.
Jake was then rushed to NICU at the Lancashire Women and Newborn Centre at Burnley General Teaching Hospital where he was stabilised.
Rebecca recalls: “Jake didn’t cry when he was born and I kept saying: ‘Why isn’t he crying?’
“After being used to hearing a baby cry at birth, it was horrendous.
“I had to be stitched up and have my blood pressure brought down so it was five hours before I got to Burnley to see Jake.
“Dr Andrew Cox came to see us at NICU and he was amazing. He talked us through what was happening and explained everything really well.
“They had cooled Jake down straight away to prevent further damage or swelling to the brain as he had been starved of oxygen.
“They could not say how he would be until they had warmed him back up. We could not hold him for three days as he was on the cooling mat and he was on medication as they thought he was having seizures.
“We finally got to hold Jake on day four and he immediately started rooting for a feed so I fed him.”
However, things took a turn for the worse when Jake developed a severe gut infection which isn’t normally seen in full-term babies.
He was very ill and was on high doses of antibiotics and nil by mouth for eight days.
Rebecca says: “Jake wanted feeding and just cried. But he couldn’t have it as it would have made him worse.
“After eight days, he was allowed one ml every two hours and this was gradually built up.”
Rebecca says by expressing milk for Jake with the support of NICU staff, it made her feel she was doing something positive for her baby.
She explains: “The staff were fantastic and they trained me how to tube-feed Jake.
“When you have a baby in intensive care, it is very difficult as there are so many things you can’t do that it can almost feel like they are not your baby.
“But expressing milk made me feel like I was doing something positive for Jake and once they were able to up his milk, he gradually got better.”
Rebecca remembers looking at Jake in NICU and thinking how big he seemed compared to the other babies and she wants people to know it isn’t just premature babies who end up in NICU.
She says: “One of the biggest shocks was that Jake was a lot more poorly than Alexis who was born nine weeks early.
“A lot of people think that with full-term babies everything is going to be fine, but that is not always the case.
“When I looked at Jake in his incubator, compared to most of the babies in NICU, he filled it and looked big.
“But Jake was actually a lot more poorly than some of the tinier babies.”
Jake was in hospital for 27 days and was able to go home with his family in October 2016.
He is now one and is doing brilliantly and hitting all his milestones.
Rebecca says: “Jake is a little star and he is walking, running, climbing up steps and shouting after his sisters.
“The doctors are really happy with his progress and say you would never know what he has been through.”
Rebecca is grateful to all the staff at NICU, not only for the way they cared for Jake but for the whole family.
She says: “The NICU staff were really open with visiting and we could take the girls in and they were fine to be around Jake’s ventilator.
“Isabella went in and put her hand on the incubator and said: ‘Hello beautiful boy’ and Alexia sang nursery rhymes to him.
“I think it is great the way NICU staff allow siblings to be involved too.”
Even though Rebecca wasn’t able to start feeding Jake herself until 25 days, through expressing she was able to establish her milk.
Rebecca says: “I had expressed so much milk that we had two freezers full and when I started feeding Jake myself, I knew I would not need it all.
“I managed to donate 17 litres of milk to the milk bank so it could go to help poorly and premature babies.
“My breastfeeding is still going strong now.”
Rebecca is full of admiration for the care and treatment provided at NICU.
She says: “The facilities are amazing and all the team support you in any way they can.
“Jake was born full-term but was born with breathing difficulties and was very poorly and ended up in neonatal.
“But now he is incredibly well with no ill effects of his traumatic start to life.
“We want to thank everyone who looked after Jake and supported us as a family.”
Dr Naharmal Soni, consultant neonatologist at NICU, East Lancashire Hospitals NHS Trust, says: “A lot of people think NICU is for tiny and pre-term babies.
“But in reality, half the babies who are admitted to NICU are full-term babies.
“Most parents expect when they deliver a baby full-term that it will be healthy and they will get to take it home that day or the following day.
“But full-term babies can be poorly, either as a result of some sort of problem at birth or from an infection which leads to breathing difficulties.
“These babies actually need more intervention than premature babies and we are lucky that at Burnley we have all the equipment and support these babies require.
“I am very happy to hear Jake is doing so well and that with the support she received with expressing, his mum is still breastfeeding as it is the ethos of the unit to support mums who want to breastfeed.”


