Perthes’ Disease
Paediatric Management Advice
What is Perthes’ Disease?
Perthes' is a childhood condition that affects the hip joint. 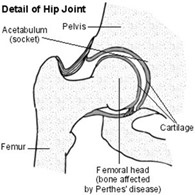
The hip joint consists of two parts: the socket (acetabulum / pelvis)
and the ball joint (the femoral head / thighbone). In Perthes, the blood supply to the top of the thighbone becomes disrupted, causing the bone to become soft and break up. This is called necrosis. It is not known why this happens and there is no known link between physical activity or other
childhood diseases and poor blood supply. It is more common in boys than in girls and usually affects children between 4-10 years old.
Who does it affect?
- Usually children who are aged between 4 and 12 years
- Boys are four times more likely to be affected than girls
- Each year, about 1 in 10,000 children are affected
- It usually only affects one hip, but both hips are affected in about 1 in 7 children
Will my child need treatment?
In many cases, the top of the thigh bone in the hip joint regrows and remodels back to normal, or near-normal. The hip joint then returns to normal and is able to work as usual. However, this can take two or more years after the condition first starts. Even after this time, there may be some stiffness remaining in the hip and there is an increased risk of arthritis in later life. The aim of treatment is to promote this healing process and ensure the hip joint heals and regrows in the correct position.
What are the symptoms of Perthes’ Disease?
The symptoms usually develop gradually over a period of time. The first indication that a child may have Perthes' disease is when they develop a limp. The affected hip is often but not always painful. The symptoms may include:
- Pain can be felt in the affected hip and also in the groin. Referred pain can also sometimes be felt in the thigh and knee.
- Limb shortening may occur in the affected side compared to the unaffected side.
- Limping is often developed and can gradually become worse over a few weeks.
- Stiffness and reduced range of movement occurs in the affected hip as the hip becomes more damaged. Hip flexion and abduction are the movements most affected.
- Muscle wasting occurs as the affected leg can’t be used normally and the muscle becomes weaker. You may notice that the affected leg appears thinner than the unaffected leg.
Important signs and symptoms to look out for.
If your child experiences any of the following symptoms, please seek further urgent medical advice:
- Swelling or bruising, not improved by elevation or rest
- Regular or constant night pain
- Leg deformity if this follows a traumatic injury
- Loss of sensation or persistent pins and needles / numbness in leg
- There is a sudden deterioration of function or movement.
- There is a sudden onset of an unexplained limp.
- Pain that does not settle with rest or reduction of activity
- Increased temperature, feeling hot and shivery may indicate an infection
- Redness and heat at hip, knee or ankle may indicate an infection
- Inability to walk on the leg
Only continue to read if you have none of the above symptoms
Treatment and management of Perthes'
Treatment and management of Perthes' depends on individual findings and X-rays, and will focus on specific symptoms. Your orthopaedic consultant will be able to advise on the most appropriate protocol / plan as well as weight-bearing status.
This may include:
- Rest
- Pain relief (analgesia)
- Limited activity / modified activity
- Specific exercises to maintain strength and mobility
- Walking aids such as crutches
- Reviews / reassessments
Your Physiotherapist will work closely with your consultant to ensure the treatment / management plan is safe and individual to each patient’s findings.
What are the long term effects?
Although more than half of children with Perthes' will return to their normal level of activity, some children may need additional reviews under Orthopaedics. Your orthopaedic consultant will advise on any reviews and re-assessments needed to track longer term progress and/or changes.
What can help?
- Swimming and cycling are recommended as this keeps the joint mobile without putting pressure through the joint.
- Pain relief medication may reduce pain, but you need to discuss options with a pharmacist or GP.
- Avoiding activities that lead to direct impact through the joint e.g. running, trampolines.
For more information, please refer to Perthes Disease - Parents Guide
Perthes Disease - Parents' Guide - STEPS Charity
If you need any further information or you feel that you need further intervention please contact the Paediatric Physiotherapy department on: 01282 803587 or email paeds.physiotherapy@elht.nhs.uk


